Hysterectomy

From 1994–1999 the overall hysterectomy rate for United States female civilian residents was 5.5. per 1,000 women. During this time period, the overall rate of hysterectomy remained fairly stable. While rates of vaginal hysterectomy remained stable, laparoscopy assisted vaginal hysterectomy (LAVH) more than doubled. Hysterectomy rates were highest in women aged 40–44 years. The three conditions most often associated with hysterectomy were uterine leiomyoma ("fibroid tumors"), endometriosis, and uterine prolapse.
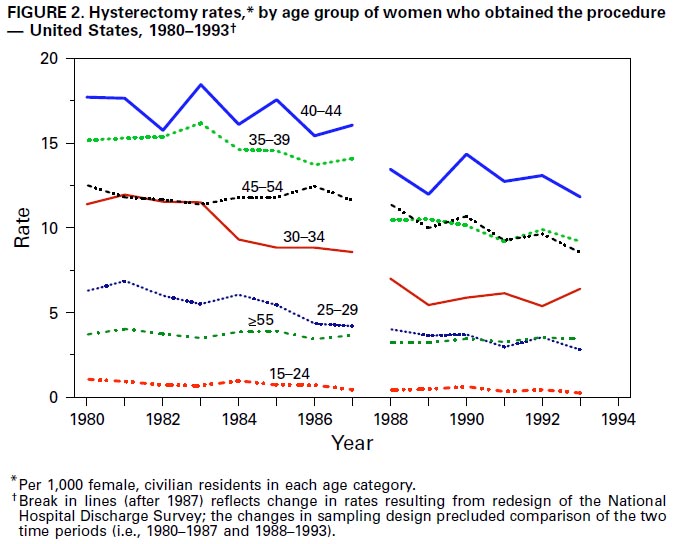
Frequency of Hysterectomy in the United States, 1980–1993
|

Women at High Risk for Hysterectomy
- From 1980 through 1993, rates of hysterectomy differed by age.
- Each year, rates were highest among women aged 40–44 years and lowest among women aged 15–24 years.
- Of all hysterectomies, 55% were among women aged 35–49 years.
- Hysterectomy rates also differed by geographic region.
- From 1988 through 1993, almost twice as many women received hysterectomies in the South (6.8 per 1,000 women) as in the Northeast (3.9). The average annual rates were 5.5 in the Midwest and 4.9 in the West.
- During 1980–1993, the average age of women who had a hysterectomy was 47.7 years in the Northeast, 44.5 in the Midwest, 44.0 in the West, and 41.6 in the South.
- Annual rates did not differ significantly by race.
Conditions Associated with Hysterectomy
- During 1988–1993, the three conditions most often associated with hysterectomy were uterine leiomyoma ("fibroid tumors"), endometriosis, and uterine prolapse.
- Among women less than 30 years of age, the conditions most frequently associated with hysterectomy were menstrual disturbances and cervical dysplasia. Among women aged 30–34 years, endometriosis was the most frequently associated diagnosis; among those 35–54 years, fibroid tumors; and among women 55 years and older, uterine prolapse or cancer.
Hysterectomy Surveillance
CDC compiles information on hysterectomies by using data from the National Hospital Discharge Survey. This survey, which collects data on discharges from United States hospitals, provides population-based estimates of U.S. hysterectomy rates. Data from national hysterectomy surveillance can be used to increase understanding of the relative public health importance of the conditions that lead to hysterectomy, identify changes in clinical practice, and assist in setting biomedical research priorities.
Alternatives to Hysterectomy: New Technologies, More Options
More than 1 in 4 U.S. women will have a hysterectomy by the time they are 60 years old, according to the Centers for Disease Control and Prevention (CDC).
A hysterectomy--removal of the uterus--can be a life-saving operation for women with certain types of cancer or uterine hemorrhage. It can also improve the quality of life for thousands of women each year who experience abnormal uterine bleeding and noncancerous growths of muscle tissue in and around the uterus (fibroids), or the falling of the uterus from its normal position into or outside of the vagina (uterine prolapse).
When the ovaries are also removed, a hysterectomy can relieve the pain of endometriosis--the growth of the tissue lining the uterus (endometrial tissue) outside the uterus.
The United States has one of the highest rates of hysterectomy in the world, with about 5 out of every 1,000 women each year having the operation, according to the CDC. Other industrialized countries show lower rates; in England, for example, the rate is less than 3 per 1,000 women annually. In Norway, it's less than 2 in 1,000.
Some are concerned that many hysterectomies are done unnecessarily in this country. "There are some cases where hysterectomy is the only option, for instance, for some types of cancer," says Anthony Scialli, M.D., director of the obstetrics and gynecology residency program at Georgetown University Hospital in Washington, D.C. "But I think we perform too many hysterectomies. It's a matter of American gynecologists being accustomed to performing a hysterectomy and American women being accustomed to getting one--based on their mother or other female relative having one. The one thing in favor of a hysterectomy is that it works for abnormal uterine bleeding--but it should be the last step, not the first step."
Of the more than 600,000 hysterectomies performed on American women in 1999, more than one-third of them were to treat fibroids or abnormal uterine bleeding.
Today, women have other options--new medications, technologies, and procedures--to treat noncancerous uterine conditions. Some of these less invasive procedures translate into lower risk, quicker recovery, and less expense. And some preserve the ability to get pregnant, unlike hysterectomy.
However, these procedures also have the disadvantage inherent with any new treatment--the lack of data demonstrating long-term safety and effectiveness. "But it's never a bad thing for a woman to ask a doctor for alternatives," says Scialli. "She should ask, 'What other options are there to manage this problem and what are the pros and cons?'"
Abnormal Uterine Bleeding
In women younger than 30, most hysterectomies are done to treat abnormal uterine bleeding. Abnormal uterine bleeding can occur as frequent, irregular and unpredictable bleeding, lengthy menstrual periods, bleeding between periods, or a heavy flow during periods. This bleeding may be caused by hormonal imbalances, growth of endometrial tissue into the wrong place, fibroids, or other conditions. And sometimes the bleeding has no identifiable abnormality associated with it.
However it occurs, abnormal uterine bleeding is an inconvenience, and it can be accompanied by painful cramping. It can also be exhausting, embarrassing and--when it results in anemia--dangerous.
After diagnosing the cause of bleeding, doctors usually turn to medications as the first therapy for treating abnormal uterine bleeding. Some estrogens and progestins are approved by the Food and Drug Administration to treat abnormal uterine bleeding in certain circumstances. Although the FDA has not approved oral contraceptives to treat abnormal uterine bleeding, some doctors prescribe them for this purpose. As with other approved medications, doctors may prescribe oral contraceptives "off label" for an unapproved use if, in their professional judgment, a patient will benefit from them.
"Ninety-five percent of abnormal bleeding associated with or without fibroids can be controlled with birth control pills," says Scialli. However, oral contraceptives may not be effective in reducing bleeding to acceptable levels in some women.
For some who experience abnormal uterine bleeding, a viable alternative to hysterectomy can be endometrial ablation. This procedure--a minimally invasive surgery that uses electrical energy, heat, or cold to destroy the endometrium--may minimize or even stop this bleeding. But the results may not be permanent. "Within 10 years, most women will have some degree of menstrual bleeding return, but not heavy bleeding," says Scialli.
The early techniques of endometrial ablation, introduced in the 1980s and still practiced by many gynecologists, are also known as "operative hysteroscopy" because they use a hysteroscope (a thin, fiber-optic tube for viewing) with an attachment to destroy tissue. The attachment may be a "rollerball" or wire loop through which electrical heat travels to remove (resection) the endometrial lining. After the uterus is filled with fluid to enlarge it for better viewing, the surgeon moves the rollerball back and forth across the lining or uses the wire loop to shave off the tissue. Potential risks of this ablation method include infection, perforation of the uterus, cervical laceration, and absorption of large volumes of fluid (fluid overload) that can lead to death.
In 1997, the FDA approved ThermaChoice, the first non-hysteroscopic ablation device to treat excessive uterine bleeding (menorrhagia) due to benign (noncancerous) causes. In 2001, the FDA approved three more similar devices. These devices are to be used only in women who have not yet reached menopause and whose childbearing is completed.
"Each type of ablation represents a simpler surgical procedure for doctors compared to traditional operative hysteroscopy," says Colin Pollard, a biomedical engineer and chief of the ob/gyn devices branch in the FDA's Center for Devices and Radiological Health. "All of the technologies have some things in common, but each delivers energy differently and each offers different feedback mechanisms to the doctor during the procedure."
The ThermaChoice Uterine Balloon Therapy System, manufactured by Gynecare, a division of Ethicon Inc. of Somerville, N.J., consists of a balloon that is inserted through the neck of the womb (cervix) and into the uterus. Through a catheter connected to a controller console, the balloon is inflated with fluid filled with sugar (dextrose) solution and heated to 188 F (87 C) for eight minutes to destroy the uterine lining.

Picture of the Gynecare System, a balloon attached to a catheter, which is connected to a small metal controller console.
The first of the three newer devices--the Hydro ThermAblator manufactured by BEI Medical Systems Inc. of Teterboro, N.J.--delivers hot salt water (saline solution) into the uterus through a tube inserted into the cervix. The hot water destroys the uterine lining in about 10 minutes. The doctor uses a hysteroscope for viewing the uterus during the procedure.

Picture of Hydro ThermAblator, an injecting device attached to a tube.
The second device--Her Option Uterine Cryoblation Therapy System made by CryoGen Inc. of San Diego--uses a probe capable of producing temperatures down to minus 148 F (minus 100 C) at the tip. This extreme cold is applied to the tissue for 10 minutes to freeze and destroy the uterine lining. Ultrasound is used to guide and monitor the procedure.

Picture of Her Option System, a simple probe.
The third device--the NovaSure Impedance Controlled Endometrial Ablation System manufactured by Novacept of Palo Alto, Calif.--uses a metallic mesh triangular electrode that is expanded out of a slender tube into the uterus. A gentle suction brings the tissue into close contact with the triangular electrode, which delivers electrical current to the endometrial tissue, causing its destruction in about 90 seconds. With this method, there is no hysteroscope or ultrasound, so the doctor cannot view the uterus during the procedure.

Picture of NovaSure System, a slender tube witha metallic mesh triangular attachment on the end.
Not For Everyone
Endometrial ablation is not advised for women who want to have children, and it is not a form of birth control. "Doctors must tell the patient she should still maintain contraception," says Pollard. "If she does get pregnant, it will be a very high-risk pregnancy." If pregnancy were to occur, the cells left lining the uterus may not be adequate for a fetus to attach and grow within the uterus.
The ThermaChoice balloon method has the longest track record of the newer, simpler ablation techniques. A three-year study of this device and one-year studies of the ablation devices approved this year--the Hydro ThermAblator, Her Option, and NovaSure--showed similar rates of effectiveness and were comparable to the effectiveness of operative hysteroscopy (such as the rollerball technique). They all reduced or stopped bleeding in 70 percent to 80 percent of the women tested.
Unlike a hysterectomy, the newer endometrial ablation procedures can be performed with local anesthesia. Ablation is usually done in the hospital on an outpatient basis; however, some women remain overnight to treat the severe abdominal pain they may experience. Most women are able to return to their regular activities several days later.
Common side effects after the procedure include nausea, vomiting, and a vaginal discharge that can last from days to weeks. "Expect to have bleeding up to four to six weeks," says Malcolm Munro, M.D., a professor and gynecologist at UCLA. "With ablation, you are traumatizing the surface whether you use electrosurgery, or burn it or freeze it."
Complications of ablation are rare, but may include blood loss requiring a transfusion, perforation of the uterus, or unintended damage to other internal organs.
Newer approaches to endometrial ablation are currently under investigation; these use other energy sources, such as laser and microwave, to destroy the endometrial tissue.
A Personal Choice
A woman must decide what she expects from a treatment for abnormal uterine bleeding. "Women need to know that articulating their problem is important for treatment," says Munro. "With abnormal bleeding, the desired outcomes vary. Some women want no period, some want a predictable period. Some want to slow the bleeding, for others pain is more important than volume. Some want to maintain their ability to get pregnant. Some don't want scars; some don't care about scars. Time off is a consideration. All of these factors are impossible for a doctor to aggregate for the patient. The woman has to make the decision."
Many women are satisfied with the outcomes of their endometrial ablations. But others, like Melissa Otto of Minneapolis, are disappointed.
Otto's hormonal introduction to womanhood--when she was 12--was frightening. Shortly after the onset of menstruation, her monthly period became very heavy and lengthy. By the time she was 14, Otto was extremely anemic from the blood loss. "The doctors told my parents not to worry--that eventually I'd regulate and have a normal period. They said 'Let's just treat the anemia for now.'"
But Otto's bleeding was no more regular by the time she reached her 20s. Medical tests ruled out fibroids and other abnormalities. Despite trying many different types of birth control pills prescribed by her doctor, her periods continued to get heavier. They came about every 23 days and lasted for 12 to 13 days. Otto spotted during the 10 days a month she wasn't bleeding heavily.
In desperation, Otto tried hormone injections, homeopathic remedies, chiropractic medicine, blood-building supplements, and acupuncture. Nothing worked.
In May 1999 when she was 31, Otto had an endometrial ablation. Her doctor used a laser to destroy the endometrial tissue. After five weeks of watery discharge and spotting, Otto's periods resumed and became frequent and lengthy once more.
In July 2000, Otto checked into the hospital for a second endometrial ablation--this time a balloon ablation. Four weeks later, her period returned--a little lighter--but still long.
After 20 years of problem periods, a dozen different doctors, hormone treatments, two ablations, and a bout of cervical cancer along the way, Otto had had enough. In March 2001, she had a hysterectomy, and Otto says that she is very happy with the results.
Fibroids
Uterine fibroids may be a cause of abnormal uterine bleeding. About 30 percent of women between 25 to 45 are diagnosed with fibroids, according to the federal Agency for Healthcare Research and Quality.
For unknown reasons, fibroids are diagnosed in black women two to three times more frequently than in white women, and fibroids account for about twice the number of hysterectomies among black women than among white women, according to the CDC. About 200,000 hysterectomies each year are performed in the United States to treat fibroids.
Also called myomata or leiomyomata, fibroids can vary from microscopic size to the size of a melon, and no one knows what causes them.
Most fibroids do not cause symptoms and require no treatment other than regular monitoring by a physician. But some fibroids can cause heavy bleeding, debilitating pain, or both. If fibroids press on the bladder or bowel, they can cause frequent urination, constipation, painful bowel movements, and hemorrhoids.
Large fibroids may cause an enlarged uterus, resulting in a protruding abdomen. "When the uterus reaches the size of a melon, a doctor would most likely recommend a hysterectomy," says Dena Hixon, M.D., a gynecologist in the FDA's Center for Drug Evaluation and Research. No treatment other than hysterectomy can guarantee that uterine bleeding or fibroids won't recur.
Treatment Options
|
There are medications that will temporarily shrink fibroids. If heavy bleeding accompanies the fibroids
and causes anemia, a doctor may prescribe an injection that temporarily stops estrogen production for up
to three months before surgery. Most fibroids are stimulated to grow by estrogen, and without it,
fibroids usually shrink. These injections, called gonadotropin-releasing hormone (GnRH) agonists, act by
causing a sort of medical menopause, says Hixon. "These are drugs with significant risks and side effects
that are most appropriately used when other common alternatives are inadequate or not appropriate for the
individual." Because of their significant side effects, including loss of bone density, hot flashes, and
mood swings, the FDA has approved GnRH agonists for use only for three months. Without surgery, the
fibroids are likely to regrow after the drug is stopped.
Women with fibroids that cause pain, discomfort or bleeding have surgical options to hysterectomy. These include surgically removing only the fibroids (myomectomy), cutting off the blood supply to the fibroids (embolization), and shrinking the fibroids using electric current (myolysis). Myolysis is not currently widely used, and no long-term studies on safety and effectiveness have been done on this procedure. The most appropriate treatment for each woman will depend on the size and location of the fibroids, the severity of symptoms, and future childbearing plans. |
Sampling can be done by dilation and curettage (D&C) or by endometrial biopsy. D&C is a procedure that involves dilating the cervix and scraping the uterine lining. In an endometrial biopsy, a thin hollow tube is inserted through the cervix and into the uterus. Cells in the uterine lining are pulled through the tube by suction and later tested in a lab.
Uterine sarcoma, a rare cancer, cannot be diagnosed by testing samples of endometrial cells. Nevertheless, sampling is recommended to check for other cancers or disease before treating fibroids or abnormal uterine bleeding.
Myomectomy
A myomectomy is a surgery to cut away the fibroids without removing the uterus, so that a woman can maintain her ability to bear children. "It's major surgery and has the same disadvantages as hysterectomy as far as pain, disability, and scarring are concerned," says Scialli. "But if a woman wants to get pregnant, myomectomy is currently the method with the best track record." A myomectomy tends to weaken the uterine wall; children born after the procedure may need to be delivered by cesarean section.
In some cases, a myomectomy may be a more complicated procedure than a hysterectomy. "After you remove the fibroids, you have to reconstruct the uterus," says Lyons.
Myomectomy can be performed in several different ways, depending on the size and location of the fibroids. In a laparotomy, a surgeon can go into the uterus through an incision in the abdomen. In another approach, a laparoscopy, the surgeon inserts a telescope-like instrument (laparoscope) through the navel and inserts other instruments through very small incisions in the abdomen. Scialli does not generally recommend a laparoscopic myomectomy for women having a subsequent pregnancy because it may weaken the uterine wall more than a myomectomy done through a larger abdominal incision.
Another method of myomectomy involves using a hysteroscope and small surgical instruments inserted into the uterus through the cervix to cut out the fibroids. Sometimes, the surgeon uses a special type of hysteroscope called a resectoscope. This instrument has a built-in wire loop and uses electrical current to cut out the fibroid. Even after a myomectomy, fibroids can still be a problem, says Scialli. "I've seen patients who never have fibroids return and patients whose fibroids recur every bit as badly within a year."
Uterine Fibroid Embolization
Uterine fibroid embolization (UFE)--also called uterine artery embolization (UAE)--is a minimally invasive procedure that blocks the arteries carrying blood to the fibroids. Because the procedure is performed by a specially trained physician called an interventional radiologist, a woman should first be examined by a gynecologist, says Lyons. The gynecologist will take the patient's medical history and perform tests to rule out any problems that may be causing the bleeding and that would require a different treatment.
In the procedure, which is done under local anesthesia, the radiologist threads a small tube (catheter) from the groin into the uterine artery. The radiologist then injects a dye into the artery and views moving X-ray images on a monitor to see the flow of blood to the fibroids. Very small particles, called embolic agents, are slowly injected through the catheter to the uterine artery in order to block the blood supply to the fibroids. (See "Uterine Fibroid Embolization.") A clot forms around the particles, which are about the size of grains of sand and are usually made from plastic (polyvinyl alcohol) or gelatin sponge.
"Uterine artery embolization is a procedure that doctors have been doing as long as 20 years, but not specifically for uterine fibroids," says the FDA's Pollard. "The procedure has been used for postpartum hemorrhaging and to stop bleeding when treating some kinds of cancer."
Since the mid-1990s, the use of uterine artery embolization to treat fibroids has grown. According to the Society of Cardiovascular and Interventional Radiology, more than 10,000 procedures have been done worldwide, of which about 8,600 were performed in the United States. Three deaths have been reported.
Although the FDA has not cleared the UFE procedure for general use, it is being studied in FDA-approved clinical trials. "It is not a trivial procedure and is not without risks," says Pollard. "And we're not sure how those risks weigh up against drug therapy, myomectomy, and hysterectomy." Potential risks include infection, ovarian failure leading to early menopause, and expulsion of the fibroid from the uterus at a later date, requiring another procedure. Additional risks include leakage of the embolic particles out of the blood vessels, complications from radiation exposure, blood clotting in the veins of the inner thigh or leg (deep vein thrombosis), blockage of an artery in the lungs (pulmonary embolus), and death.
Unlike a hysterectomy, UFE leaves the uterus intact, with the potential for childbearing. However, current research is lacking on the ability to become pregnant and carry a baby to full-term, says Pollard.
More Data Needed
Compared to hysterectomy, minimally invasive surgeries to treat uterine problems are relatively unknown territory. "While these are promising technologies, we don't have data on their long-term safety, effectiveness, and fertility," says Amy Allina, program director of the National Women's Health Network, a nonprofit women's health advocacy organization in Washington, D.C. "It's a matter of choice. I don't consider any of these options perfect for everybody."
Peri-Menopause/Menopause/Hysterectomy Basic Saliva Hormone Test
Nevertheless, women today do have a multitude of good options to choose from to maintain their health, says Lyons. "Information about these options is out there but individuals must access this knowledge in order to take advantage of these choices. Be proactive and know all you can know to best serve yourself and your families."